Home
Boater's Supplies
Buy Safety & Flotation equip.
Buy Marine GPS & Electronics
Sea Survival articles:
This section contains medical information with the specific needs of the castaway in mind. It focuses primarily on the survival situation in which a minimal amount of medicines and equipment (if any) is available, and it addresses those emergencies and problems that are most likely to occur. The emphasis is on a lay man’s diagnosis and improvisation of treatment, rather than the application of medicines and dosages normally prescribed or recommended by a physician. How effective you are concerning medical treatment and the usage of drugs is your decision entirely, since a comprehensive coverage of either subject does not fall within the scope of this guide. This is not a complete medical summary, nor is it meant to be a substitution for a professional medical guide. Rather, it is designed to effectively illustrate the symptoms and treatment of a variety of physical maladies to which the castaway is most commonly exposed.
SURVIVAL FIRST AID
In the survival situation, the definition of first aid must be expanded to include final aid. Since professional medical treatment is not normally available in an emergency situation, all injuries must be dealt with in a complete and final manner.
Minor Injuries
First aid treatment for minor injuries is designed to “contain and treat” the injury in order to minimize the possibility of complications and to promote speedy recovery.
Major Injuries
First aid when applied to major or massive injuries is the attempt to neutralize and stabilize the injury until proper medical treatment can be found.
In the survival situation the understanding and early recognition of medical problems is crucial for two primary reasons:
• The lack of adequate drugs, medical services, and equipment.
• The fact that many maladies can be avoided altogether or at least greatly minimized by early detection and treatment. Dehydration, hypothermia, and shock, for example, are grave threats to the exposed or injured castaway and early recognition of each of these vital to their treatment.
HEAT EXHAUSTION
Heat exhaustion (also called heat prostration) is caused by a loss of water and salt from the body. Heat exhaustion results from exposure to high temperatures, and not necessarily just from exposure to direct sunlight. Cases of heat exhaustion are common among persons working in hot environments, such as engine rooms or furnace rooms, as well as outdoors in hot or humid conditions.
Heat exhaustion differs considerably from heatstroke, even though both conditions represent a failure in the body’s mechanisms of regulating heat. While heat exhaustion can lead to collapse, it is much less serious than heatstroke.
Symptoms
• Skin appears pale and clammy
• Profuse sweating
• Weakness, dizziness, nausea, fainting
• Pulse will be fast and weak
• Breathing will be rapid and shallow
• Pupils dilated
• Mild muscular cramps (heat cramps)
• Body temperature below normal
• Possible headache and chills
• Dim or blurred vision
Treatment
To normalize the circulation of blood, effective treatment must restore salt and fluid to the body.
• Place the patient in the shade, away from the heat source if possible.
• Lay the patient in a reclining position with his head slightly lower than his feet. This will increase the flow of blood to the head.
• Keep the victim warm by covering him with blankets or clothing.
• Keep the victim rested and quiet, and protect him from excessive heat and physical activity until he has recovered.
• To treat heat cramps, remove the victim from the heat source and massage the affected areas to help relieve the cramps.
HEATSTROKE
Heatstroke is a much more dangerous condition than heat exhaustion and should be considered a medical, emergency.
Heatstroke occurs when the body’s cooling system no longer functions, because of exposure to extremely high air temperatures or the combination of excessive humidity and moderately high temperatures. When the temperature of the blood rises, the body’s primary source of heat loss (the evaporation of sweat) ceases to function. The body’s temperature gradually increases, and if not stopped, will eventually lead to circulatory collapse and deep shock, or death.
It is vital to be able to recognize the early stages of heatstroke so that corrective measures can be taken while the process is still reversible.
Symptoms
• Sudden onset, with possible fainting, dizziness, convulsions or delirium.
• Skin is hot, flushed and dry, typically red in color. Absence of sweat.
• High body temperature; high blood pressure and generalized weakness.
• Strong and rapid pulse.
• Possible muscular twitching and visual disturbances.
• Headache, nausea, and vomiting.
Treatment
The onset of heatstroke requires immediate treatment to reduce the body temperatures in order to prevent possible brain damage or death. The most effective treatment is a liquid cooling bath. The victim should be placed in a bath of cool water.
A cooling bath can be a dunk in the ocean. (If shark is present, then saturate the victim and his clothing with cool sea water to bring his temperature down.)
If a cooling bath is not possible, move the victim to a cool or shaded area, have him lie down and looser’ any constricting clothing.
Cover the skin with wet, cold towels, cloths, or blankets, changing them frequently as they get warm; or sponge the victim with cold water. Continue to cool down the victim until his temperature drops.
The body temperature should be taken every ten minutes if possible. The cooling process must be continued until the body temperature falls below 101°F (38.3°C). If a thermometer is not available, feel the skin from time to time, and watch for signs of improvement such as: lower temperature, presence of perspiration, normal facial color, and slower pulse and respirations.
It is important to massage the skin vigorously during the cooling procedure. This will prevent the constriction of blood vessels and will stimulate and accelerate the return of “cooled” surface blood to the overheated core of the body.
IMMERSION FOOT/TRENCH FOOT
Immersion foot and trench foot are both local cold injuries resulting from prolonged exposure of the lower extremities to waters just above freezing temperatures. Contributing factors include inactivity of the extremities, and restriction and immobilization of the limbs. Blood circulation is reduced, causing the feet and toes to become stiff, numb, discolored, and swollen. In acute stages, flesh may die and amputation of the foot or leg might become necessary.
It is important to diagnose this type of cold injury early, because the beginning stages cause numbness rather than pain, and can gradually and almost unnoticeably lead to acute stages.
Treatment
Treatment is limited. Terminate the exposure to the cold water as quickly as possible. Attempt to keep the feet dry and warm. Keep the legs in a horizontal position to increase the circulation.
FROSTBITE
Frostbite is the most serious of local injuries that can result from exposure. Frostbite is the freezing of a body part in which tissue destruction occurs. Superficial frost bite (sometimes referred to as frost nip) occurs when only the surface of the skin becomes frozen. In this instance, the surface will feel hard, but the underlying tissue will be soft and “spongy” when depressed. This type of frostbite can be treated by re-warming the area and ending exposure.
Typically, frostbite begins on the small areas of the extremities (nose, fingers, ears), but is capable of spreading into larger areas. If the freezing process continues and develops into “deep” unthawed frostbite, the areas will become completely hard and cannot be depressed. At this stage, the thawing process must be started quickly. Only time will enable you to determine the serious degree of frostbite that has occurred.
Symptoms
Frostbite is not very painful in the early stages. The patient will typically feel a numb, tingling sensation. It is important to recognize the onset of frostbite to prevent it from causing serious problems.
The effects of serious frostbite can be seen before they are felt. In cases of prolonged exposure:
• Ice crystals in the skin tissue cause the area to appear white or grayish-yellow in color.
• In 12 to 36 hours, blisters will appear on the surface and underlying tissues. The area will appear very swollen and red when it thaws, and gangrene and necrosis (loss of tissue) will follow.
Treatment
Immediate re-warming is the best treatment. Treat it as soon as possible, but introduce heat very gradually, to prevent the onset of shock.
There are two types of rapid re-warming techniques:
• The wet technique is the quickest and therefore the most ideal. After terminating exposure, place the victim in a bath of heated water (104° to 107°F or 40° to 42°C in temperature). This will most efficiently accomplish the warming process. If you do not have a thermometer, test the water with your finger or elbow to make sure it is not too hot.
• The dry warming technique is the use of blankets, the sharing of body heat or heat sources. This technique will take 3 to 4 times longer than wet warming.
There are certain things that should never be done when treating frostbite:
• Never try to forcibly remove frozen clothing (shoes, mittens, etc.). Place the frozen piece of clothing in lukewarm water until it becomes soft, and then gently remove it.
• Never attempt to thaw a frozen body area by exercising it.
• Never let the victim stand on frozen feet. This will only complicate problems by damaging tissue and breaking the skin.
• Never massage or rub frozen body areas. This may cause further tissue damage.
• Never soak frozen limbs in kerosene or oil.
• Never expose frozen body parts directly to an open flame or fire.
• Never use water over 111°F (44°C) to re-warm a patient or body part.
• Never thaw a frostbitten body area until you are sure that it will not be frostbitten again. The refreezing of a body part can result in irreparable damage.
GANGRENE AND AMPUTATION
Gangrene, briefly defined, is the localized death of soft tissues caused by loss of blood supply. It may follow an injury such as severe frostbite, where the freezing of tissues has cut off blood supply for prolonged periods. Gangrene may also develop when tourniquet pressure has been used to seal off the blood flow of an infected or bleeding limb for such an extended period of time that the tissues have died from lack of blood supply.
Gangrene provides an ideal condition for bacterial growth and the spread of infection to the “living” parts of the body. It is extremely dangerous and if allowed to go untreated, can be fatal.
Gangrene can be either dry or wet in appearance, is painful, and produces offensive-smelling liquid. If an injury becomes dark and hard, gangrene must be suspected. Advance stages of gangrene can be remedied only by amputation. (Note: The conditions, procedures, and ramifications of amputation are lengthy and complicated and are beyond the scope of this guide.)
BLEEDING
The human body contains approximately 6 quarts of blood. The loss of anymore than one pint is considered both dangerous and life threatening. Hemorrhaging is when there is excessive bleeding and loss of blood.
Hemorrhaging of a major blood vessel (arm, neck, or thigh) can cause death in a matter of minutes. It is, there fore, vital to immediately stop or control any severe bleeding in a wounded person.
Only the restoration of breathing takes priority over the control of hemorrhaging in an emergency.
External bleeding can be from arteries, veins, capillaries, or a combination of all three, and should be treated first by direct pressure to the wound. If profuse bleeding continues, a tourniquet must be applied. (See section on Tourniquets later in this section).
Internal bleeding occurs when vessels are ruptured and blood leaks into body tissue. This sometimes results from blows to the body or diseases (such as bleeding ulcers).
Remember: A little blood goes a long way! Things usually look worse than they are.
Control of Bleeding
The methods to control bleeding include:
Direct Pressure. The simplest method is to apply direct pressure with the hand to the wounded area. Use a sterile pad or clean cloth. Pressure will promote the formation of blood clots, compress shut the open blood vessels, and prevent germs from contaminating the open wound.
Elevation. If bleeding persists, try elevating the wounded area to utilize the force of gravity. This will also lower blood pressure.
Pressure Points. Apply pressure to the artery that supplies the blood to the wounded area. This technique should be used only if direct pressure and elevation of the limb are not successful (Fig. 10-1).
Tourniquet. Use a tourniquet as a last-resort mea sure only if all other methods fail.
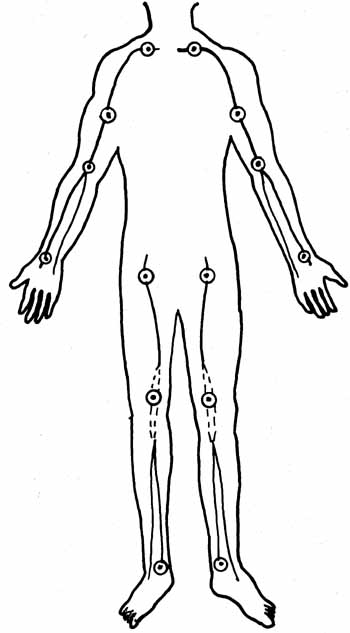
Fig. 10-1 Pressure points in the human body.
Tourniquet
A tourniquet is a constricting band used to stop arterial bleeding (spurting vessels) of an extremity. It is a last-resort measure and should only be used when all other techniques have failed to control the excessive flow of blood.
The danger involved in applying a tourniquet is that all blood flow beyond the point of application is blocked. This can be extremely dangerous. By cutting off circulation for a prolonged period of time, tissue destruction can occur from lack of blood and oxygen. If tissue dies, removal by amputation might be necessary.
Caution should be exercised when applying a tourniquet. If applied too loosely, it will not stop the bleeding; if applied too tightly, it can severely damage muscle, nerves, and tissue. Remember, the purpose is to stop the bleeding.
Improvising a tourniquet can be accomplished by using materials such as cloth, towels, tubing, belts, or anything that will provide a band around the limb. The band should ideally be at least 1 to 2 inches wide and long enough to encircle the limb twice (Fig. 10-2).
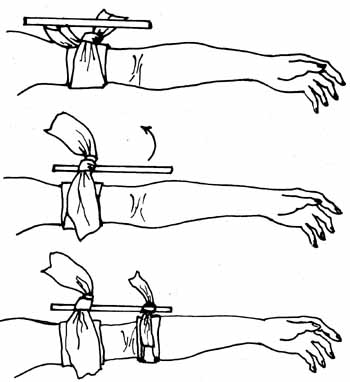
Fig. 10-2 The illustrations indicate proper methods for applying
a tourniquet.
Applying a Tourniquet
• Place the tourniquet between the body trunk and the wound, (between the heart and the wound) approximately 2 to 4 inches above the injury. In the case of injuries just below the knee or elbow, it is advisable to apply the tourniquet above the knee or elbow. Never apply a tourniquet directly over a wound or fracture.
• Wrap the tourniquet material loosely around the limb and tie a simple knot (square knot).
• Lay a piece of wood or similar item over the tourniquet band and secure it with a single knot.
• Twist the stick several turns until the bleeding stops, but not tighter. While a tourniquet will stop the major spurting (hemorrhaging) of blood, some time may be required for the smaller veins to drain. Don’t feel compelled to stop the minor bleeding. You may be tightening the tourniquet too much.
• Attach or fix the stick to the limb to maintain pressure. Secure the stick in place using another bandage, tape, or piece of cloth. (At this point, treat for shock and attend to the wound.)
Once the tourniquet has been properly applied, there are several points to keep in mind:
• Keep the treatment area as warm as possible.
• Never cover a tourniquet. The application of a tourniquet has been forgotten on occasion; and if the patient is unconscious or heavily sedated, he may not be aware of the treatment. (A forgotten tourniquet can be tragic.)
• Attach a note on the patient’s clothing or elsewhere in an area that is clearly visible. Describe the location of the tourniquet and the date and time of its application.
Do not loosen or remove the tourniquet that was applied to stop the bleeding in the case of an amputated limb. It should be removed only under the advice and supervision of a physician.
Remember, permanent uninterrupted application of a tourniquet will result in death of the limb. Periodic loosening of the tourniquet will allow blood to flow into the limb long enough to keep the limb and tissues alive. The dangers of loosening a tourniquet (periodically or other wise) are serious. Additional loss of blood occurs, which could promote shock and other complications. If the tissue is dead and infection or gangrene has set in, the loosening of the tourniquet will allow dangerous bacteria to flow into the “healthy” body.
A complete medical book should always be included in a yachtsman’s library.
SPRAINS
Sprains are a common injury, especially in the wrist and ankle areas, caused by the extreme twisting or pulling of a joint and ligaments. Sprains can be quite painful and easily confused with a bone fracture.
Symptoms of Sprains
• Swelling
• Bruising
• Pain
Treatment
Apply cold wet packs, when available, to help relieve the pain and swelling. If possible, elevate the injured part. A splint can be applied if the sprain is severe.
FRACTURES
A fracture is a cracked or broken bone, usually occurring in the limbs of the body. There are two types of fractures: compound and simple.
Compound Fractures
A compound (open) fracture is considered a serious injury since the broken bone has pierced the skin and is protruding from the limb. There is constant danger of infection and contamination.
Treatment
• Scrub with soap and boiled (but cooled) water.
• Remove any foreign matter that is easily removable.
• Do not attempt to force the bone end back into place.
• Apply a sterile dressing and immobilize the fracture with a splint.
• Use antibiotics to prevent infection, and offer pain relievers if available.
Simple Fractures
A simple (closed) fracture is diagnosed when apparent symptoms indicate a broken bone. There is no open wound to speak of, but certain appearances in the limb, indicate a break: shortening or lengthening in the limb, deformity, crookedness, or perhaps the sound of a bone snapping. Sometimes only intense pain, swelling, or discoloration will be evident.
Treatment
• Do not move the fractured limb. Any improper movement can cause damage to tissue, nerves, and blood vessels.
• Apply a splint, if there is no obvious gross deformity, to immobilize the fracture. Padded splints are best, a pillow or bulky blanket will work.
• Apply a firm and steady pull in the direction of the normal axis of the bone, if very deformed, until alignment looks fairly normal. Do this as soon as possible after the injury. The pain will be greater if you wait to do it.
• Make sure that sensation (to pin prick) and circulation (pink fingers and toes) are present.
• Apply a firm compressive dressing if there is a large amount of swelling with elastic bandages and elevate the extremity for at least 2 hours.
Splints
If a splint has not been included in your first aid kit, one can be improvised by simply fashioning a device that will keep the limb immobile. Boards, sticks, fishing poles, even magazines or dry newspaper, when folded properly, can work.
If no materials are available to improvise a splint, the limb can sometimes be secured to another limb, such as in the case of tying together two legs, fingers, or toes. Apply the splint snugly to prevent any slipping or further injury, but not so tightly that it prevents blood circulation in the limb (Fig. 10-3).

Fig. 10-3 Splints for fractured or broken bones.
The splint should extend beyond both the joints above and below the injured limb. In the situation of a boat or raft on the ocean, it may be necessary to secure the injured limb, once the splint is applied, to the torso. This will help prevent movement of the limb caused by the raft’s motion.
Recently a new type of splint has come into use.
Made of a lightweight, transparent plastic that can be inflated by mouth like a balloon, in a matter of seconds. It can be stored in a small space.
DISLOCATIONS
Dislocations are usually obvious. Fingers and toes can be easily popped back into place with firm traction. After repositioning, splint the area in the normal resting position (natural curve) for at least 1 to 2 weeks. An injured toe can be splinted by taping it to an adjacent good toe with cotton between the toes.
For a dislocated shoulder, take pain medicine. Lie prone with the injured arm hanging over the edge of a platform far enough above the floor to allow you to hold a suspended bucket. Slowly fill the bucket with water as tolerated. This traction will eventually cause the shoulder to go back into place with a definite snap and pain relief.
INFECTIONS
Symptoms
• Red, painful, skin, often with red streaks.
Treatment
• Scrub with soap and water 2 to 4 times daily.
• Apply warm wet compresses.
• Elevate if the infection is on an extremity.
Urinary Tract Infection
Symptoms include burning on urination, blood in urine, urge to urinate frequently, or pain over kidney area, and fever. Take lots of fluids to keep the kidneys flushed, and appropriate medicine if available.
BURNS
Treatment
• First degree burns (red skin only): Cold soaks for 15 to 20 minutes. No other treatment is usually necessary.
• Second and third degree (skin blistered or sometimes white or charred): Cover area with mild soap (Phisohex) and wash gently. Follow this with a sterile non-adherent dressing. Change dressing periodically. If fever develops, take antibiotics.
WOUNDS
Wounds are generally broken down into five basic types:
Abrasion. An abrasion is an open wound caused by scraping the skin. It can be painful if the abraded area is very large. Bleeding from damaged capillaries and small veins is usually minimal.
Contusion. A Contusion is a closed, superficial wound usually the result of a blow from a blunt object. If the injury is located over a bone, there is a possibility of a fracture.
Puncture. A puncture is an open wound, usually with a small opening, and very dangerous if the object has penetrated deeply. An ice pick, for instance, would leave a small hole but could severely injure organs or cause internal hemorrhaging. External bleeding generally helps to cleanse a wound, but in the case of a puncture wound where less bleeding occurs, this cleansing process is mini mal. Therefore, the possibility of infection is greater. Possible complications include lockjaw, tetanus, or gangrene.
Incision. An incision is usually caused by a sharp object. If the wound is deep, severe damage to muscles and nerves might occur. The amount of bleeding will depend on the depth of the cut.
Laceration. A laceration is caused by a ripping action (broken glass or moving machinery). This type of wound is jagged and irregular in appearance and may bleed more freely than an incised wound.
Diagnosing Wounds
Wounds vary as to the degree of damage sustained, and are designated: superficial, minor, major, massive, and complicated. The severity of a wound cannot always be determined at first glance. A wound from a nail for example, may appear minor, but if an internal organ were punctured, it could endanger your life; conversely the mangled surface skin on a scraped knee, though relatively minor, could appear more severe than it is.
It is important to acquaint yourself with first aid procedures for both minor and major wounds in order to quickly diagnose the extent of a wound and initiate proper treatment.
The possibility of infection is present in all types of wounds, no matter how minor, and should be treated accordingly.
Treatment of Minor and Superficial Wounds
• Expose the wound. Remove clothing by cutting away or gently undressing.
• Elevate the wound, if possible. This reduces blood pres sure, swelling, and bleeding.
• Allow the wound to bleed a short while, but do not squeeze. Any squeezing may cause damage to the tissue.
• Do not disturb any blood clot that has already formed.
• Remove foreign objects and material that are easily removable.
• Take action to control bleeding by applying pressure to the wound.
• Cleanse the wound with mild soap and boiled water that has cooled. Use a rubbing stroke directed from the wound outward to minimize the chance of germs entering the wound.
• Apply an antiseptic dressing and bandage.
• Apply a splint, if the wound is near or on a joint, to keep the wound immobile.
• Watch for infection.
Treatment of Major and Complicated Wounds
Massive wounds require proper treatment to avoid complications at a later time. Pause to assess the situation fully since premature actions can aggravate the injury.
Most major wounds should be treated as follows:
• Restore respiration, if necessary.
• Stop hemorrhaging, if necessary.
• Treat for shock (See Section on Shock elsewhere on this page.)
• Remove clothing from the wound area.
• Do not move the victim until you are sure that it is safe to do so. Moving the patient improperly might induce or intensify shock.
• Stop any bleeding by using the direct pressure technique.
(The exception is any injury where either brain, eye, or abdominal contents are exposed. If this is the case, then all and any pressure should be avoided and the wound merely covered with sterile gauze until proper treatment can be applied.)
• Take necessary steps to control severe bleeding. This may include using “pressure points” or even resorting to a tourniquet.
• Do not cleanse or use antiseptics when treating massive wounds.
• Give antibiotics to the patient.
• Do not give stimulants until the bleeding has been stopped, and then only if the patient is conscious.
• Obtain medical help immediately, if at all possible. (Obviously in the survival situation, you will have to judge type of medical treatment to be applied.)
FISH-HOOK WOUNDS
Embedded fish-hooks are one of the most commonly en countered accidents at sea. The seriousness of an embedded hook depends on the size of the hook, its location, and depth.
Treatment of Fishhook Wounds
• If the fishhook is in superficial skin, use a sterile razor blade and cut down through the skin to the shank of the hook and lift it out. Avoid cutting any visible blood vessels.
• Flood the wound with an antiseptic and then bandage.
• For a deeply embedded fishhook push the hook through the skin until the barbed end comes through. Snip off the eye end of the shank (with wire cutters), then pull on the barbed end and ease out the shank (Fig. 10-4).
• Treat the wound with an antiseptic and apply a sterile bandage. ( a fishhook is in or near the eye, do not use an antiseptic.)
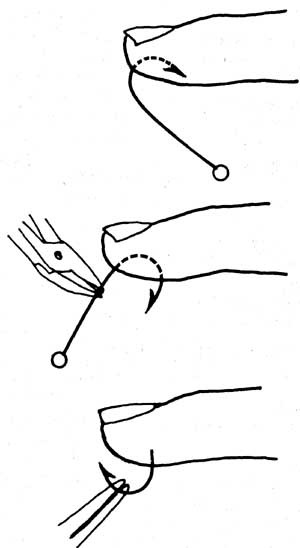
Fig. 10-4 Proper procedure for removing embedded fishhook
SHOCK
Shock results from an over-taxation of the nervous system, along with a drop in blood pressure, causing an inadequate blood flow to the brain and other vital organs of the body.
Shock varies in degree but is present, to some extent, in all injuries. Consequently, the understanding and recognition of it is important in any first aid treatment. The following section deals with injury-related shock, not electrical shock.
What Causes Shock?
Shock might follow any type of injury. The mere sight of blood can cause a person to become weak or nauseated, this is a mild form of shock usually followed by a quick recovery. Deep shock, however, may develop after severe injuries such as:
• Major crushing injuries
• Severe pain
• Fractures of the larger bones
• Great loss of blood
Shock might also result from such conditions as allergies, heat stroke, heart attack, infection, emotional stress, or poisoning (chemical or drug, and even extreme alcohol intoxication).
Types of Shock
Anaphylactic. Anaphylactic shock is an allergic shock from bee stings, Portuguese man-of-war jellyfish, or drug allergies (can be due to almost any drug).
Symptoms. Often just wheezing and a feeling of swelling in the mouth or throat. Sweating, weakness, dizziness, loss of consciousness, itchy rash, or hives might occur.
Neurogenic. The sight of blood, fear, or apprehension, causes neurogenic shock.
Symptoms. Victim might experience lightheadedness, faintness, or dizziness. Victim may be pale and sweaty.
Volume Depletion. Blood loss or severe dehydration causes volume depletion.
Symptoms. Symptoms are similar to other symptoms of shock, but the cause should be evident (bleeding, pro longed vomiting and/or diarrhea).
General Symptoms
• Clammy, pale, or cold skin. A bluish or ashen color may later develop.
• Rapid and weak heartbeat. (Pulse may be almost imperceptible.)
• Thirst or nausea.
• Shallow and rapid breathing.
• Victim may be restless, excited, apprehensive, hysterical, dizzy, or faint.
• An initially anxious expression may later change to a general dullness and a vacant, glassy stare.
Treatment
It is important to take immediate action. When treating for shock, your main objectives are to alleviate shock, shorten its duration, and prevent it from progressing or recurring.
• Eliminate the causes of shock by restoring breathing, controlling bleeding, and if possible, relieving any severe pain.
• Position the victim horizontally, lying down with the feet slightly higher (12 inches) than the head. This will in crease the blood flow to the head. In the case of a head injury, reverse this procedure so that the head is higher than the rest of the body. (Do not elevate the legs or feet if a head or chest injury is present or if there is any difficulty in breathing.)
• Lay the victim on his side to allow for drainage from the nose and mouth if he is unconscious or has severe facial injuries.
• Cover the victim, if necessary, to maintain his normal body temperature.
• Loosen any constrictive clothing and reassure the person.
• Treat the basic injury.
• Administer appropriate drug, if available.
DROWNING
The treatment for drowning encompasses basic life sup port resuscitation techniques (Fig. 10-5).
If victim is not breathing, give mouth-to-mouth resuscitation, even if the victim is still in the water. Use a floatation device to support the victim’s neck.
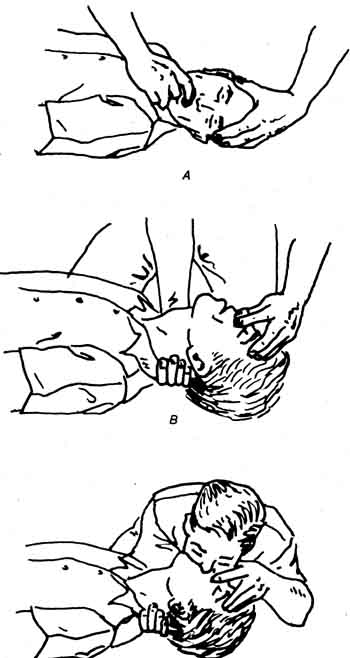
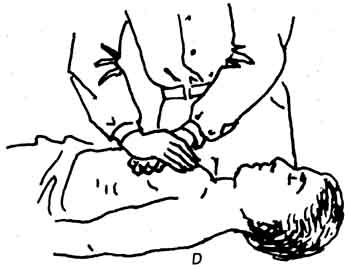
Fig. 10-5 The illustrations demonstrate the proper way to apply
CPA techniques.
To empty the stomach of a drowned victim once he is out of the water (on shore or in the raft), lay him in a face down position lifting under the stomach with your hands to force the water out. The stomach of a drowned victim usually becomes distended because of the large amounts of water swallowed.
If the victim vomits, turn his head to the side and clear out his mouth. Continue resuscitation techniques until the victim is revived.
SEASICKNESS
Motion sickness on the ocean is called seasickness. Physiologically, it results from continuous “contradictory” messages and signals being transmitted to the brain. This causes a state of “confusion” as the brain attempts to sort out the conflicting signals. Your “inner ear” balance sys ten (vestibular) is basically at odds with your “visual” reference system (the system providing information to the brain about one’s position in relationship to the horizon), thus causing seasickness.
The following elements or combinations of elements may contribute to the conflicting information to the brain:
• The ocean’s up and down motions
• The swaying and loss sensation
• The eyes’ automatic tendency to seek stationary references (horizon)
• The reaction of “position sensors” in your joints and tendons (especially the neck)
• Food, fatigue, illness, alcohol, drugs, and other individual factors may contribute.
In the survival environment, seasickness can be extremely dangerous. If vomiting occurs, vital body fluids will be lost and if water rations are low, it may mean the difference between surviving or death from dehydration. Repeated vomiting may prevent the taking of any orally administered medication. If this is the case, suppository application of medicine may be necessary.
Treatment
By nature of their absorbing qualities, small amounts of dry foods, crackers, bread, or similar foods may help to alleviate seasickness. Rest in a reclining position with the eyes closed, can aid the seasick person by minimizing the signals responsible for causing the seasickness.
BODILY ELIMINATION
A severe change of diet in the survival situation can cause chronic constipation. Some feel that this is beneficial in that any bowel movement requires body fluids and will result in the loss of precious water from the body.
Often a bowel movement will not occur for extended periods of time with no ill effects. Fresh water, if applied rectally via an enema, will aid in producing a bowel movement, but should only be administered if ample water is available. (Brackish water may be used.)
Urination should continue, although perhaps less frequently and in less quantity. When urine becomes dark in color or painful to pass, this is usually a symptom of dehydration, and is generally not harmful or unusual.
SWELLING
Swelling frequently occurs in the hands and feet. Gentle massage will help to alleviate the swelling. Joints tend to swell and become stiff and weak. Using and stretching joints several times a day will help to minimize the swelling.
BLISTERS AND BOILS
The buttocks and lower extremities may develop sores, boils, or blisters from continued exposure to wet conditions. Try to keep these areas dry, and change clothing frequently, if possible.
CRAMPS
Cramps in the limbs can occur from lack of use, loss of salt from the body, or excessive heat. Massage and knead the affected area.
DEATH
The confirmation and pronouncement of death is a medical decision that should be reserved for proper authorities when possible. Normally, attempts to resuscitate a victim should always continue until a physician arrives. In the survival situation, proper medical help may not be avail able, but nevertheless all attempts should be made to resuscitate a victim. This should be done not only for the sake of the victim, but also for the morale and spirit of the other crew members.
The will to live is the most valuable survival tool available to the castaway, and should be supported and reaffirmed at every instance. It is, however, necessary to be able to diagnose the termination of vital life signs to be fully confident that the person is deceased.
Death signs can be categorized in two basic classifications:
• Those that are apparent shortly after death (early signs)
• Those that are visible some hours or days after death has occurred; in most cases, death will be unmistakable when it occurs.
Suspecting Death
The complete absence of a heartbeat and lack of breathing for at least 20 minutes is an early sign of death. Remember that it is difficult to ascertain this without aid of medical equipment, such as a stethoscope.
Be complete in your diagnosis. Suspended animation (death trance) can result from electrical or injury-related shock. This condition produces an almost imperceptible heartbeat and pulse, a slowing down of other vital signs, and little or no trace of breathing.
When the heart stops beating, the pupils will begin to dilate within 45 seconds to 1 minute and will remain dilated, not reacting to light.
Using a mirror is the time-honored method of verification of death. By placing the mirror directly under the nose or mouth of the victim, any amount of breathing will be noticeable since the warm air of the breath will condense on the mirror.
If a mirror is not available, a light material, such as a cotton wisp can be used. If the surrounding air is calm enough, movement in the wisp can be noticed when it is held in front of the nose and mouth.
Later Signs
• A drop in body temperature. This is influenced by the amount of clothing the victim may be wearing, the air temperature, and the amount of time the victim has been dead.
• Appearance of the eyes. The transparency of the cornea turns into a milky or cloudy state and the surface be comes wrinkled.
• Rigor mortis. This is the stiffening of the muscles and general rigidity of the body. Although it is subject to variation, it usually appears within 2 to 8 hours after death and begins in the facial muscles, gradually extending to the legs. It lasts about 16 to 24 hours and will disappear in the same order as it appeared.
• Putrefecation. This is the rotting or decomposing of the body. Depending on the condition and temperature of the air, this process usually won’t begin until one day after death and not until rigor mortis has disappeared. This is absolute verification of death.
Last Rites
The body of a dead person in the survival craft must be done away with for reasons of morale and health. A decomposing body could infect those around it.
All clothing and everything of any possible value should be taken off the corpse before discharging it into the sea. Any pertinent information should be recorded. The body may float for awhile, and if your raft is adrift the body may in fact follow the craft. If this happens, it can present emotional strain, but try to retain your perspective and composure.
The following prayer may be read upon commencement of a burial at sea:
“Almighty God, our Father, from whom we come and unto whom our spirits return: Thou hast been our dwelling place in all generations. Thou art our refuge and strength, a very present help in trouble. Grant us thy blessing in this hour, and enable us to put our trust in thee that our spirits may grow calm and our hearts be comforted. Lift our eyes beyond the shadows of the earth, and help us to see the light of eternity. So may we find grace and strength for this and every time of need. Amen.”
PREV: Survival in Cold Climates
NEXT: Psychology of Survival
All Sea Survival articles
© CRSociety.net